A value-based system where healthcare providers are accountable for outcomes will benefit patients
What makes a good hospital visit? Few people might actually enjoy going to the hospital, but most can agree that a “good” visit means getting high-quality care and emerging in better health, as quickly and painlessly as possible.
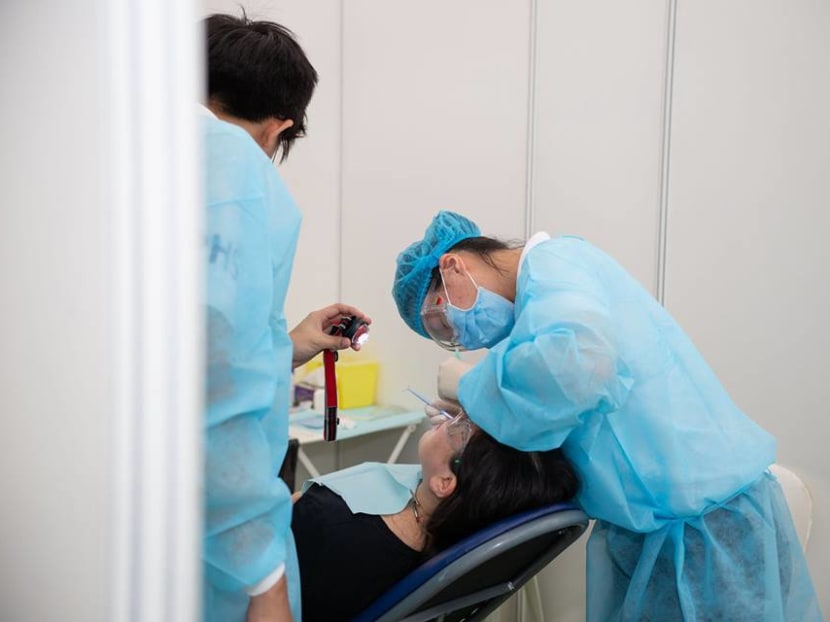
Value-based healthcare models will require strengthening metrics and evaluation and putting in place financial incentives that ensure providers are held accountable for high-quality care, positive patient experiences and good health outcomes.
What makes a good hospital visit? Few people might actually enjoy going to the hospital, but most can agree that a “good” visit means getting high-quality care and emerging in better health, as quickly and painlessly as possible.
Unfortunately, many health systems are not designed to prioritise the type of care that patients value the most — timely, appropriate and caring treatment that is effective yet affordable, in the hands of competent professionals who listen and respond to their needs.
In “fee-for-service” models, which is how most health systems traditionally operate, healthcare providers from doctors to hospitals charge for each procedure, regardless of what the outcome may be.
As payment depends on the volume of services provided, such models incentivise quantity over quality, encouraging speedy delivery at the expense of other aspects of high-quality care.
Singapore has long been recognised as having one of the world’s most effective and efficient healthcare systems, beating global average life expectancy by 12 years while ranking second only to Hong Kong on Bloomberg’s Health Efficiency Index.
However, faced with the rising demands of an ageing population and chronic diseases such as diabetes, healthcare expenditure has been growing at a rate that the Ministry of Health (MOH) describes as ultimately unsustainable.
WHAT COULD BE A SOLUTION?
Value-based healthcare is an approach to healthcare management that considers the entire patient journey – from diagnosis and treatment to after-care, and if possible, prevention – and asks, how can we design systems that focus on the delivery of health rather than health services?
Value-based models aim to fulfil this vision in multiple ways. These include strengthening metrics and evaluation, better integration of care, supporting innovations that drive efficiency, and by putting in place financial incentives that ensure providers are held accountable for high-quality care, positive patient experiences and good health outcomes.
Globally, the wave of value-based healthcare is already underway.
In the United States, the Health Care Transformation Task Force, (a non-profit industry consortium that brings together patients, payers, providers and other stakeholders) reported by the end of 2017, nearly 47 per cent of its members’ business operated under value-based payment arrangements. It has committed to a goal of increasing this to 75 per cent by the end of 2020.
Closer to home, MOH has identified value-based healthcare as an integral part of transforming the healthcare system, from planning to service delivery. A number of pioneering initiatives that support value-based healthcare are already taking place in Singapore.
For instance, the National University Health System has developed a data visualisation platform for continuous monitoring of financial and quality performance, providing a holistic and actionable view of patient care that enables teams to prioritise, initiate and evaluate projects that improve outcomes while lowering costs.
Elsewhere, pilot initiatives have been launched that aim to revisit current processes and encourage care coordination, such as hospital-to-home programmes that train multidisciplinary teams to provide home-based care instead of extending inpatient stays. This would improve patient satisfaction, reduce infection risk and free up scarce hospital beds.
As the pressure on health services continues to rapidly increase, how can we then accelerate progress towards making value-based healthcare a reality for all Singaporeans?
I recently moderated a panel at the 3rd Annual Value-Based Healthcare Seminar in Singapore, hosted by Johnson & Johnson, in which international speakers and local healthcare experts came together to highlight three interdependent and critical drivers of such progress.
These were: Rigorous and transparent data analytics to provide evidence and accountability, a payment system that rewards desired outcomes on the roadmap to change and a cultural shift that embraces innovation and collaboration.
For patients to get optimal care plans that span different healthcare services, it is necessary to have timely and accurate real-world indicators of cost and outcomes across the entire patient journey from multiple sources, such as electronic medical records, health claims and patient surveys.
For healthcare policymakers, such data will give them the ability to experiment with fail-fast pilot programmes and adapt accordingly based on measurable outcomes.
EXPLORING NEW WAYS TO PAY
Building on this strong foundation of data, we can rethink the way we pay for healthcare. In general, value-based payment arrangements seek to link compensation to patient-centric outcomes rather than the quantity of services provided.
These range from pay-for-performance models (where compensation depends on achieving pre-determined performance benchmarks), bundled payments (where a lump sum is paid for the management of a given condition, subject to quality standards) and capitation (where a fixed sum is paid per head for all the healthcare needs of a pre-defined patient population).
Speaking at the seminar, Mr Chan Beng Seng (Group Director, Healthcare Finance, MOH) described the move towards value-based financing through the introduction of bundled payments in Singapore.
In the case of hip fractures for example, a patient may have surgery as an inpatient in the acute hospital but receive post-surgical care and outpatient rehabilitation services at a community hospital.
A single fee is fixed for the “bundle” of services, with one clinical team overseeing the overall care and rehabilitation plan.
Quality measures are monitored closely along the journey, including later hospital readmissions after final discharge. When properly designed and implemented, bundled payments give all providers an explicit interest in collaborating to achieve high-value care more efficiently without compromising outcomes.
Whilst heading in the right direction, Singapore’s path to value-based healthcare is long and undoubtedly complex. It requires all stakeholders to be prepared to scrutinise their services, work efficiently and transparently, and integrate care beyond traditional silos.
This also means looking at a definition of “healthcare” that transcends the treating of the sick and includes disease prevention and the promotion of healthy living.
By continuing to embrace value-based initiatives and innovations, we can help to safeguard the sustainability of a patient-centred health system and, most importantly, continue keeping Singaporeans as healthy as possible for as long as possible.
Perhaps, in the future, the best kind of hospital visit is not having to visit at all.
ABOUT THE AUTHOR:
Dr Joanne Yoong is a visiting associate professor at the National University of Singapore’s Yong Loo Lin School of Medicine as well as senior economist and director at the Centre for Economic and Social Research East, University of Southern California.









