Understanding immunisation and why a Covid-19 vaccine is no magic bullet
Vaccines are special medications that train our immune systems to create memory cells that recognise certain bacteria and viruses harmful to us.
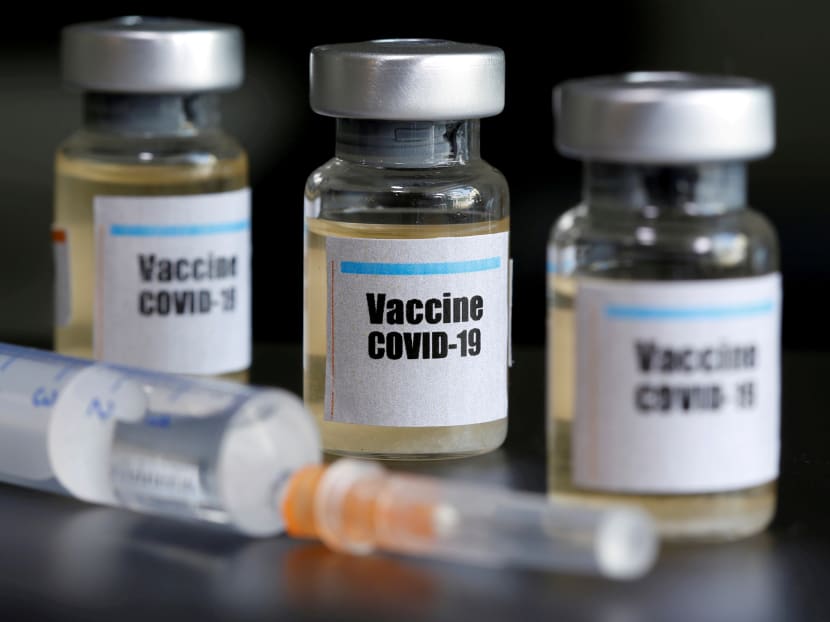
Most attention is now on the development of a vaccine for Covid-19, which will be crucial for the pandemic to end and for travel restrictions and physical distancing measures to be eased, writes the author.
Vaccines are special medications that train our immune systems to create memory cells that recognise certain bacteria and viruses harmful to us.
By rapidly mounting an immune response when challenged, these memory cells prevent the diseases caused by them.
Vaccination or immunisation is considered one of the greatest public health interventions in the world, saving millions of lives a year.
World Immunisation Week falls on the final week of April every year, and is a global campaign aimed at raising awareness and increasing rates of immunisation against vaccine-preventable diseases worldwide.
The theme this year is #VaccinesWork for All, but unfortunately, the campaign has been overshadowed by the Covid-19 pandemic.
Nonetheless, immunisations remain critical at this time, particularly those on the National Childhood Immunisation Schedule, and are rightly recognised as an essential service by the Ministry of Health during the current circuit breaker.
Doctors and nurses in polyclinics and private clinics around the island continue to provide vaccinations necessary to forestall future outbreaks of diseases such as measles and poliomyelitis.
Ironically, the vaccine that had been heavily promoted in recent years — the influenza vaccine — has become an optional one for the community during the Covid-19 pandemic.
The influenza virus spreads in a manner similar to Sars-CoV-2, the virus that causes Covid-19, and the circuit breaker measures will limit its spread.
Nonetheless, preventing the spread of influenza via immunisation will become important again once physical distancing measures are eased and society opens up.
Naturally, most attention is now on the development of a vaccine for Covid-19, which will be crucial for the pandemic to end and for travel restrictions and physical distancing measures to be eased.
At present, there are over 70 vaccine candidates in development, although only a handful have entered early phase human clinical trials.
Vaccine development is traditionally a lengthy and costly process.
It entails animal testing, three phases of human trials requiring thousands of volunteers to determine safety and efficacy, licensure by regulatory authorities such as the United States Food and Drug Administration and the European Medicines Agency (the equivalents to Singapore’s Health Sciences Authority) and large-scale manufacturing.
Because high failure rates are the norm and vaccine development can cost upwards of S$1 billion, developers typically take a linear approach, requiring each step to be passed before going on to the next.
The normal timeframe for a successful vaccine to reach the market is between six and 10 years.
For instance, a vaccine against the Middle East Respiratory Syndrome (Mers) coronavirus has just reached human clinical trials, despite having been in development since 2014.
In a crisis like the current Covid-19 pandemic, a linear approach to vaccine development gives way to one with overlapping or parallel steps.
While this will dramatically shorten the timeframe, it increases financial and safety risks. Nonetheless, even if every phase of vaccine development goes smoothly, it will be over a year before the first vaccine becomes commercially available, in view of the extremely rigorous testing required to ensure the safety and efficacy of a medication that will be used on millions of otherwise well persons.
Some have questioned the need for so many vaccine candidates, arguing that this dilutes efforts and increases costs.
However, it is important to note that no one has ever produced a coronavirus vaccine that has reached the market.
The four human coronaviruses cause the common cold — a mild disease — and there was therefore little point in investing in a vaccine against them.
No vaccine was ever developed for the severe acute respiratory syndrome (Sars) coronavirus because it quickly disappeared after a few months.
So having many different approaches and multiple shots at a Covid-19 vaccine at the beginning increases the chances of success overall.
Despite this, we need to understand that even if an effective vaccine against Covid-19 is developed, the immunity it confers may last only for a period of time rather than for a lifetime. In general, unless an infection confers lifelong immunity to survivors, it will be extremely challenging to engineer a vaccine that does so.
Infection by the human coronaviruses, just like in the case of influenza, does not result in lifelong immunity. One’s immunity wanes after several months and it is possible to develop the common cold repeatedly.
Scientists have tracked antibody levels in Sars and Mers survivors and found that on average, these drop significantly two to three years post-infection, suggesting that immunity is not lifelong for the majority of survivors.
What about Covid-19 and the Sars-CoV-2 virus?
There are still many things we do not understand about our immunological response to them.
Chinese scientists reported that a few patients with mild infection did not develop neutralising antibodies to the virus, with the implication that they could possibly be re-infected again.
Much more time is needed for observations and studies before we can be certain about the issue of immunity to Covid-19. However, given what we know about existing coronaviruses, it is plausible that immunity for the majority of those infected may at best last several years.
If ultimately we fail to develop a Covid-19 vaccine, all is not lost, as the non-pharmaceutical interventions imposed by different countries have been effective in containing the spread of the virus and minimising loss of lives, including in Singapore.
In particular, territories like South Korea and Taiwan have been able to do this without lockdowns and with minimal disruption to society. They can be role models for such a future.
If a vaccine is developed but does not offer 100 per cent protection — say, a little better than the influenza vaccine which is approximately 50 per cent — it can still be effective if a very high percentage of the population is vaccinated.
This is because Sars-CoV-2’s R0 — the number of new infections stemming from a single case — is relatively low at two to 2.5.
So vaccination can be incorporated into an overall long-term strategy, including the need for repeated vaccination every few years.
The ideal — which as mentioned is a very long shot — will be a vaccine that provides universal lifelong protection.
Even this will not eliminate Sars-CoV-2. This is because there will always be those who are anti-vaccination and others who do not respond to the vaccine, particularly those that are most vulnerable to Covid-19 — the elderly and those with suppressed immune systems.
To reiterate, many routine immunisations are still critical even during the pandemic, and children especially should complete their courses of vaccinations.
While great effort has and will go towards the development of a Covid-19 vaccine, it is good to understand that this will very likely not be a magic bullet that will eliminate the virus from the world.
However, even a somewhat effective vaccine will be very helpful in limiting the threat of Covid-19 in the future.
ABOUT THE AUTHOR:
Associate Professor Hsu Li Yang heads the Infectious Diseases Programme and is co-director of the Leadership Institute for Global Health Transformation at the Saw Swee Hock School of Public Health, National University of Singapore.









