The Big Read: Apathy, complacency — the worst enemies in Singapore’s war against diabetes
SINGAPORE — To 26-year-old Asraf Mustaffa who recently stepped into the working world, it is clear why diabetes is a ticking time bomb in Singapore.
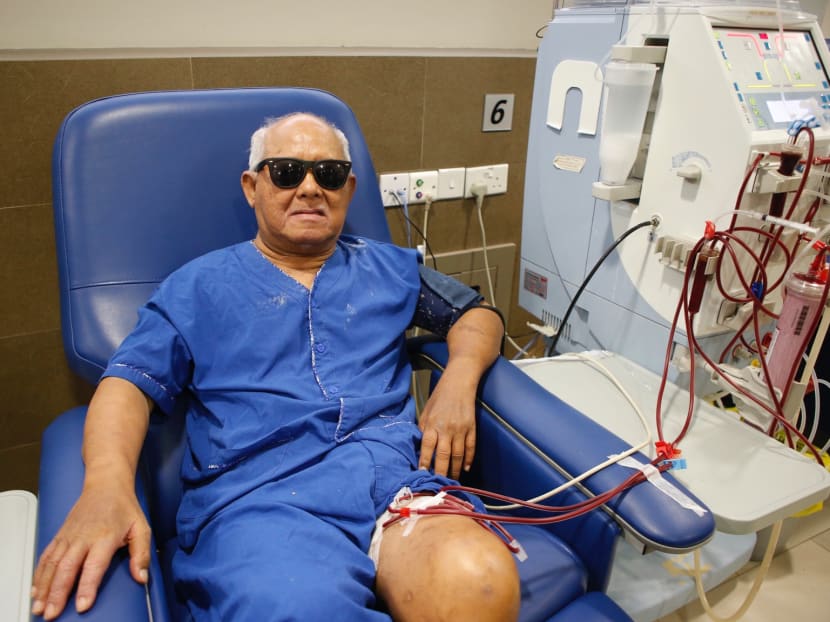
Mr Mohamed Dollah, 71, an amputee with impaired vision looks back at his lifestyle with some regret, having lost the sense of independence and freedom. Photo: Najeer Yusof/TODAY
SINGAPORE — To 26-year-old Asraf Mustaffa who recently stepped into the working world, it is clear why diabetes is a ticking time bomb in Singapore.
Most of his peers are leading an “out-of-whack” work lifestyle characterised by eating on the go and turning to fast food for convenience, while sitting hours on end in an air-conditioned office, relying on a snack or two to get through the high-pressure environment.
Mr Asraf knows all about the harm of a “haywire diet” and lifestyle: He was diagnosed with diabetes at 13 years old, following years of bingeing on sweetened juices and traditional delicacies.
Turning to his peers’ unhealthy lifestyle, the business graduate said it was only a matter of time before diabetes “stops them in their tracks on whatever they are doing”.
Statistics show that he is not too far from the truth. Diabetes strikes one in nine Singaporeans today, and its prevalence almost triples with age – just second behind the United States among the developed countries.
Painting a grim picture at his National Day Rally (NDR) speech last week, Prime Minister Lee Hsien Loong warned that this “invisible” but deadly disease is increasingly posing a risk to Singaporeans, especially the younger ones.
In April last year, Health Minister Gan Kim Yong declared a “war on diabetes”. More than a year on, the message has not quite sunk in, as Mr Lee acknowledged. Noting that some Singaporeans have wondered why diabetes would be a fitting topic at the NDR, he said: “It is precisely because you are not worried, that I am worried. It is precisely because many people do not take diabetes seriously, that it has become a serious problem.”
An average of about 1,200 diabetics (nearly four a day) undergo amputations every year. Slightly more than half of these patients are Chinese (53 per cent). About a quarter (27 per cent) are Malays, while 14 per cent are Indians, the Ministry of Health (MOH) said in response to TODAY’s queries.
Singapore’s major lower extremity amputation rate is 28.5 per 100,000 population - much higher than all the Organisation for Economic Co-operation and Development (OECD) countries, based on data published in 2015.
Israel, which tops the list of OECD countries, has a rate of 15.9 per 100,000 population. At the other end of the spectrum was South Korea (2.4 per 100,000 population).
An MOH spokesperson reiterated that early treatment of foot ulcers could prevent infection and subsequent amputation. The ministry is working to provide more support services, such as diabetic foot screening, to the general practitioners through the Community Health Centres and upcoming Primary Care Networks. A pilot programme is also underway by the National Healthcare Group Polyclinics to carry out “more targeted and intensive foot surveillance” for at-risk patients, manage early ulcers and infections, and facilitate fast-track referrals to hospitals.
Many fatal health complications, such as heart attacks, stroke, and kidney failure can also be traced back to organ damage due to diabetes.
Diabetes has been described as the “silent killer”. Unlike an infectious disease such as Hepatitis B where one can be diagnosed as positive or negative, diabetes exists on a “spectrum,” said Dr Chan Tat Hon, a medical doctor who conducts lifestyle modification programmes and training for patients with chronic lifestyle-related conditions such as diabetes.
“Instead of asking the question ‘Am I a diabetic’, it should be useful to ask ‘How diabetic am I?',” said Dr Chan.
ATTITUDES
Overall, there is a sense of apathy and complacency towards the disease among the Singapore general population, medical experts say.
The most worrying age group is those under 40 years old, said Prof Chia Kee Seng, dean of the National University of Singapore (NUS) Saw Swee Hock School of Public Health.
“Unfortunately, at that age, they are more concerned with pursuing wealth, very often at the expense of their health,” said Prof Chia. “By the time they enter their 50s and 60s, they start to be more concerned about their health but the damage caused by neglect in the first 50 to 60 years would be more difficult to reverse.”
Often, younger people think they are “invincible” and often dismiss their diabetes risk as they think they are “fully active” with an “ideal body weight”, when they ought to be careful, warned Assoc Prof Subramaniam Tavintharan, who is a senior consultant endocrinologist at Khoo Teck Puat Hospital. He sees a “very heterogeneous” group of patients, including those who actively exercise and are not obese.
There is no one isolated reason that increases the risk of diabetes but a whole host of factors that stack up, making it a complex disease to ward off, the experts explained. These stem from weight, high blood pressure and cholesterol, activity level, genetics and age, among other factors.
“Unfortunately, quite a lot of people seem to develop this notion that only the fat and lazy develop diabetes, but it is not true,” said Dr Subramaniam. “Because of that, (a lot of diabetics) feel uncomfortable sharing their condition with their friends.”
THE (UNHEALTHY) TYPICAL S’POREAN LIFESTYLE
For audio-visual support staff Mr Sufiyan, 24, the “quickest and most convenient” lunch option while he is at work is to use a delivery app to order some fried chicken. He would snack on cookies or potato chips to sate the occasional hunger pangs. By the time work ends at 11pm, he “just wants to go home and sleep”, said Mr Sufiyan.
Back in his student days, he seldom drank plain water but would down Red Bull, and chill out almost every night with friends at McDonald’s with some ice cream or fries. Healthier food options such as a bowl of salad would not appeal to him, as he felt that it does not provide enough sustenance. While he admits his lifestyle is not ideal, he said: “Sometimes you want to care, but (mostly) you can’t be bothered…There’s just no time as we just have to make a living.”
During the NDR, Mr Lee noted that two decades ago, Singaporeans ate on average, 2,100 calories every day. By 2004, it went up 2,400 calories a day, equivalent to two extra ice cream scoops daily. By 2010, this was 2,600, amounting to an extra scoop of ice cream with topping.
For Lasalle College of the Arts student and freelance theatre practitioner Anne Lee, 23, she is “not a huge fan” of fried food and she eats plenty of vegetables. Nevertheless, it is common for her to have a hearty supper of prata and nasi briyani together with her crew mates at a popular Indian-Muslim eatery after their shows end at around 10pm. This nightly routine sometimes lasts “two weeks up to one month”, she said.
Ms Lee, whose father has diabetes, said: “(There’s this mentality) that I’m still young... I still can avoid (getting diabetes) by cutting down and making changes (later).”
Exercise also becomes a low priority for many Singaporeans when they have to spread their time thinly between work and caring for children and aged parents, for example.
After plying the roads all day, taxi driver Mr Hartono, 56, who has diabetes, said he is just too exhausted to set aside time to exercise - a far cry from his younger days when he “loved sports” such as squash and gym and would go swimming with his “kakis.” “Life in Singapore is not easy, (it’s) so fast paced. We all work, work, work… (Who talks) about exercise? No work, no money. No money, no talk,” he said.
Nevertheless, thanks to Mr Lee’s NDR speech, some Singaporeans are sitting up and taking notice of the problem.
One of them is marketing executive Ang Xin Jie, 25, whose family also has diabetes. She said that after NDR, she talked about the issue with colleagues, and started to get concerned even though she has generally led a healthy and active lifestyle.
Ms Ang said she makes a “conscious effort” to eat and exercise properly, such as opting for a dish with more vegetables, ordering unsalted fries and bubble tea at a quarter of the usual sugar levels. She also squeezes in time for pole dancing lessons and weekly runs. However, she admits that she is often guilty of not sleeping enough. Occsionally, she gets off work at about 11pm. “It doesn’t help that I’m a night owl so I usually go to bed at 1am to 2am,” she said.
According to the experts, later marriages also pose a risk. Older pregnant women have an increased risk of contracting gestational diabetes mellitus (GDM), which is glucose intolerance at the onset of pregnancy, said Dr Matthias Toh, a public health physician at the National Healthcare Group (NHG). This is because glycemic control - the body’s ability to keep blood glucose in check - also deteriorates with age.
Especially troubling is how nearly one in five pregnant women here (17.6 per cent) tested had GDM – a rate that is almost double the 9.2 per cent rate in the United States, according to a study by the National University Hospital and the KK Women’s and Children’s Hospital published in September last year.
Even though the diabetes symptoms improve or go away after delivery, the disease is “ever present” as a high number of mothers afflicted with GDM will develop diabetes later, said Singapore Medical Association president Dr Wong Tien Hua.
Up to half of women with GDM develop diabetes within five years post-delivery, said Dr Gabriel Yee, the assistant honorary secretary of the Diabetic Society of Singapore. Babies born to diabetic mothers have an increased risk of obesity and developing diabetes when they are older, the expert noted.
FOR THE NEEDY, DIABETES COULD BE HARD TO MANAGE
In the past, diabetes had sometimes been described as a “rich man’s disease”. But globally, there is growing recognition that it is increasingly a “poor man’s disease”. Diabetes prevalence is higher in poor countries than in rich countries, due to a combination of factors such as poverty, poor education, poor food quality and high levels of physical inactivity.
In Singapore, sustaining a healthy lifestyle can be more difficult for needy diabetic patients such as Madam Vapkin Venkitachalam, 56. At the market, she would pick ikan bilis over the more expensive fresh fish any day.

The former kitchen porter often gets food rations - which include items such as a pack of white rice, packets of instant noodles and a bottle of oil - which do little for her condition.
Brown rice, which is the healthier option, costs more than white rice. Supermarket chains NTUC FairPrice and Sheng Siong have said they will offer discounts on brown rice.
Mdm Vapkin, who lives in a Toa Payoh rental flat, requires insulin jabs daily and has been coping with diabetes for more than 40 years, “Hospital gives (the injections) free... They all help me. ‘Makan’ (food in Malay) who want to help? I eat white rice. Nobody help me,” she said. She suspects her 29-year-old son has diabetes too but he has refused to go for a body check-up. He binges on soft drinks and chocolates daily, to the extent that his urine “attracts ants”, Mdm Vapkin said.
She added that exercise is “a luxury” for her son who works 12 hours a day, six days a week as a stock-keeper.
Retiree Chumiah Kamalruddin, 69, who is diabetic, receives the same food rations as Mdm Vapkin. She told TODAY she has more pressing worries than eating well, such as finding the money to pay a S$600 hospital bill which is due by the end of this month.
Another diabetic Mr Devadas Nagalindan, 56, who works 12-hour shifts as a security guard, said he wolfs down white bread and butter at lunchtime because it gives him “a full stomach”.

But carbohydrates - which many blue collar workers rely on to give them the energy for work - is precisely what causes blood sugar to rise, said Ms Julie Seow, who coaches people with diabetes at Touch Community Service’s diabetes support arm.
“Carbohydrates is not only the cheapest across all food groups, it is also comfort food,” she noted.
Just as obesity has a strong correlation with low income, diabetes too has the same link - considering the disparity in the access to better quality food such as organic food, or less-sugar variants of different brands, said Singapore Management University sociology professor Paulin Tay Straughan. “All the prescriptions that we give to keep diabetes at bay - less sugar, less fried food, exercise more - is easier for somebody with (the) means,” she said.
But as a society, there is a tendency to “blame the victim”, where the lower-income diabetic are unfairly stereotyped as a group for “being stubborn” about switching to healthier options, Prof Straughan said.
Nevertheless, NUS sociologist Tan Ern Ser pointed out that the well-to-do “have their own expensive carbohydrate-rich foods such as ice cream, puddings, cakes and pastries… maybe durians too”.
“When we adopt a class perspective to explain the incidence of diabetes, are we suggesting that the poor have no choice but to eat carbohydrate-rich food?” said Dr Tan. He suggested the problem could lie in a “lack of awareness of the danger of a carbohydrate-rich diet”, instead of a lack of access to healthy food. “Healthy food can be affordable too. But if not affordable, then the voluntary welfare organisations (VWOs) should consider giving healthier food options, with sponsorship from businesses,” he said.
ALL ROUND EFFORTS
Already, community groups and VWOs are doing their bit to tackle the problem of poor nutrition among the needy.
The Food Bank Singapore, for instance, started distributing healthier food bundles under its Project Eat Better campaign in March last year, supplying beneficiaries with items such as brown rice vermicelli, extra virgin olive oil, oats and fruit and vegetable packs.
But The Food Bank Singapore Chief Food Officer Nichol Ng said that in order to go beyond “the usual staples” of rice and oil donations, her organisation needs to continuously advocate for donors to provide a greater variety of products.
The Food Bank Singapore supplies food items donated by the public to more than 200 VWOs and Family Service Centres, which then distribute these items to low-income households that include the elderly and those living in rental flats.
Noting how some of the needy do not have refrigerators at home, Ms Ng said community fridges could go some way to alleviate the problem. With support from the Tampines Town Council, the Tampines North Citizens’ Consultative Committee had started a community fridge project in January to help provide food for needy residents.
A Fei Yue Community Services spokesperson noted that lower income or disadvantaged groups and communities tend to have “limited access to better resources”. While the group “appreciates donations from do-gooders”, it has also encouraged givers to be “more intentional and purposeful” in giving help, with regards to the providing healthier food for the needy.
Lakeside Family Services executive director Teo Tee Loon, whose organisation distributes food rations such as rice and cooking oil to needy clients, said it also provides “supportive counselling” to clients with health issues including diabetes and high blood pressure. The counselling includes constant encouragement for the beneficiaries to “keep up with their treatment and dietary disciplines”. Lakeside Family Services also conducts annual health and nutrition talks, as well as cooking demonstrations where people learn how to prepare “simple, healthy and economical meals”.
Hoping that food companies can chip in with more brown rice donations, Mr Teo said: “We would be very glad to partner with companies which could help us provide better health and nutrition education to our clients, as well as healthier food rations.”
Ms Ng said it is a common misconception that eating healthy means eating expensive, Her group has set up a YouTube channel among efforts to start a “sharing community” of economical recipes.
The community efforts come on top of several government initiatives announced by the MOH earlier this year, such as enhanced subsidies from Sept for the Screen for Life programme which allows eligible
Singaporeans to undergo recommended screening tests for diabetes, high cholesterol, colorectal cancer, and others.
MOH will also roll out a diabetes risk-assessment tool, which is a self-administered questionnaire targeted at those aged 18 to 39. The public sector has also started catering healthier food at all its events and training courses, such as more whole-grain options, fewer deep-fried items, and fresh fruits.
A COMPLICATED ‘WAR’
Diabetes is a “wicked problem” that requires “constant adjustments and innovations” in efforts to combat it, said Prof Chia.
Socio-cultural, psycho-emotional, behavioural, economic, and genetic factors are all intertwined with the disease, he noted. “We should avoid oversimplifying the issues and turning to quick and easy solutions for immediate results,” said Prof Chia. Waging a war against diabetes has to be done from multiple battlegrounds, he reiterated.
Instead of putting labels on what is “unhealthy” and “healthy” food, and overwhelming people with a list of what they should or should not eat, Dr Chan said it is more important to nudge people into the right direction by focusing on how to “eat right for yourself and to eat better than what you are already eating”. For example, when diabetic patients have a “grain-heavy” diet or consume more meat when they eat out for “better value”, he advises them to start “bit by bit” by putting more vegetables on their plate. Healthier food does not come at the expense of taste, he added.

Dr Chan, who used to work full-time in the kitchen at The Bento People which he started in 2014, said that to entice people to eat better, he used to create healthy dishes with a twist, such as quinoa fried rice, quinoa lemak, olive vegetables red rice and Thai green curry cauliflower.
Recalling how a customer once brought her husband to the eatery as a surprise, Dr Chan said: “(The moment) the husband heard the word ‘healthy’, he literally bolted out of his seat and ran out without even looking at the menu… I had a big laugh about it, but that’s what we’re up against.” Shaping good dietary habits has to start from the cookhouses and kitchens, he added.
Ms Seow felt that current campaigns which emphasises prevention could alienate those who already have diabetes. “Maybe this very war is creating a stigma here… Everyone is trying to avoid and fight diabetes. If you are diagnosed, it is as if you have lost the war,” said the 60-year-old, a former lawyer who was diagnosed with Type 1 diabetes when she was 27 years old.
Type 1 diabetes is generally associated with a genetic predisposition, while Type 2 diabetes tends to be linked to more modifiable lifestyle factors such as obesity, living a sedentary existence and having unhealthy eating habits.
Ms Seow felt that Singapore needs more prominent champions, such as United Kingdom Prime Minister Theresa May who has Type 1 diabetes, and Hollywood star Tom Hanks and American Idol judge Randy Jackson who have Type 2 diabetes. These public figures can quash the stigma that diabetes is a “death sentence”, she added.
Diabetes screening efforts should also be stepped up, and a structured diabetes prevention or lifestyle intervention programme could be introduced at a national level, said Dr Bee Yong Mong, a senior consultant at Singapore General Hospital’s department of endocrinology. NHG’s Dr Toh said there could more efforts to help identify people with “pre-diabetes”, or those with borderline high blood glucose levels.
Going head to head with the disease can prove a “labour intensive” and costly battle, said Dr Goh Kian Peng, a senior consultant at the Saint-Julien Clinic for Diabetes and Endocrinology in Mount Alvernia Hospital.
A Saw Swee Hock School of Public Health study estimated that Type 2 diabetes cost Singapore more than S$1 billion in 2010, and this could soar to beyond S$2.5 billion annually by 2050, if current trends continue.
Diabetics interviewed by TODAY agreed that more can be done to address the problem.
Madam Christine Lee, 64, suggested having television shows where food bloggers and nutritionists look for healthier food at various eating places including hawker centres and restaurants. “I often get diabetic buddies calling me up to say, ‘Hey, Christine, I’m at the hawker centre. What should I eat?’ So every time we say yong tau foo, or fish soup, which can sometimes be not healthy as the soup base can be full of sugar or MSG (monosodium glutamate),” she said.
More nightly mass exercise sessions could also be organised at parks and shopping malls to cater to office workers, said Madam Juliana Lim, 48, an IT and administrative staff.
Mr Asraf believes that ultimately, a strong network of family and community support for those at-risk as well as those diagnosed with diabetes is crucial, because the war on diabetes is also a psychological one.
He recalled how he was rushed to the hospital about a decade ago, after he decided to stop injecting insulin. “(My family always) kept talking about no money for this and that, so I thought, ‘what if I just stopped (injecting)... their (burden) might stop,” he said.
Nursing student Lee Lay Xin, 19, who has Type 1 diabetes, said she had to be warded for a week when she was 10. This was after she was afraid to tell her aunt that she did not have enough insulin vials to last the night, for fear that she may not allow her to stay over at her place.
Touch Diabetes Support’s Ms Seow said: “Diabetes cannot be seen as a personal fight... (it) is firstly a family affair.” Adding that a supportive family and great doctors who are readily available are important factors, she said: “The family eats what (the diabetic) can eat, and plan meals around what everybody can enjoy.”











