Initial results of study find no community spread of Covid-19 in Singapore as of end-March
SINGAPORE — New studies carried out by researchers have found that there has been no widespread community transmission of Covid-19 here up until the end of March.
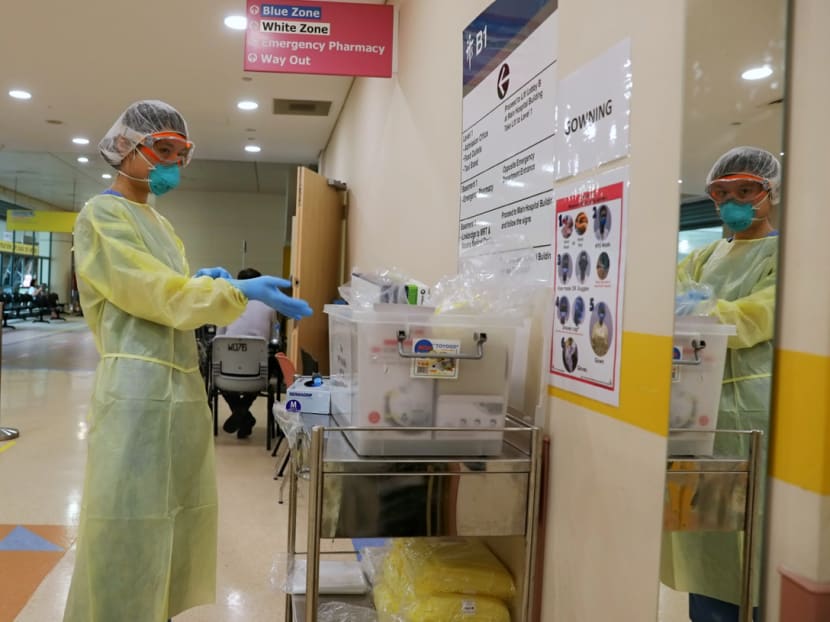
A staff member of Tan Tock Seng Hospital's emergency department putting on protective gear. A new study suggests that the measures taken to keep healthcare workers safe have successfully ensured that they do not get infected with the coronavirus.
SINGAPORE — New studies carried out by researchers have found that there had been no widespread community transmission of Covid-19 here up until the end of March.
Professor Leo Yee Sin, who chairs the Covid-19 research workgroup that commissioned the studies, said this suggests that contact tracing efforts have been successful in identifying most of the cases of infection in Singapore, and few have fallen through the cracks.
The preliminary findings of the study were released on Wednesday (April 29) during a press conference held to give more information on the three studies.
The research workgroup was set up in January to study and come to a greater understanding of Covid-19 transmission in Singapore.
Its members are health experts from across the public healthcare institutions, the Ministry of Health, the DSO National Laboratories and the Agency for Science, Technology and Research (A*Star).
Dr Mark Chen, head of research at the National Centre for Infectious Diseases (NCID), stressed that these initial results were obtained in the tail-end of March and early April, before the rapid rise in cases from the foreign worker dormitory clusters.
More research is being done in the coming weeks to assess the current levels of exposure in Singapore, he added.
There are three seroepidemiological studies involved — they primarily examine blood samples to understand the spread of infection and to detect the antibodies produced in response to a disease before vaccination.
The human body produces antibodies in response to an infection and these antibodies remain in the blood for some time even after the patient has recovered.
Seroepidemiological testing has been used before to determine the level of community transmission for other infectious diseases, such as human immunodeficiency virus (HIV).
These tests for Covid-19 were carried out around late March and focused on three groups within the population:
Healthcare workers
Close contacts of Covid-19 patients who live in the same household
Individuals who had visited clinics or hospitals for matters unrelated to Covid-19 and whose leftover blood samples were used to measure how widespread the infection is in the community.
The following are what the preliminary findings show:
1. Cases in the community
For the third group who saw doctors for non-Covid-19 reasons, 268 leftover blood samples were collected from children and 506 from adults of all ages.
None of them had antibody levels that met the criteria to be considered positive for Covid-19, which suggests that no widespread community transmission was present as of the last two weeks of March.
“However, the not-so-good news here is that our entire population remains very susceptible because there is not enough community immunity at this time that we can detect in Singapore,” Prof Leo said.
Still, Dr Chen said Singapore can rely on other strategies to contain the virus, such as testing patients early and isolating them as soon as they are infected to prevent further transmission.
He added that effective contact tracing can also help to catch asymptomatic infections.
“All this depends on the community in Singapore doing its part,” he said, adding that each person has to maintain good hygiene and be socially responsible.
This will work in tandem with the efforts made by the public sector agencies, he said.
2. Healthcare workers
The study of more than 1,000 healthcare workers found that there was no evidence that the workers had contracted the disease even though about half of them had to be around Covid-19 patients frequently.
This suggests that the measures taken to keep healthcare workers safe have successfully ensured that they do not get infected, Dr Chen said.
For instance, healthcare workers caring for Covid-19 patients are required to put on the full set of personal protective equipment at all times.
The workers who enrolled for the study come from various departments and job scopes in the healthcare sector, including administrative staff members.
Associate Professor Raymond Seet, senior consultant at the department of medicine in the National University Hospital and one of the researchers leading the study, said that those who care for infected patients are from various departments as well, such as in the emergency room and the isolation wards.
Therefore, the sample is fairly representative of the healthcare worker population in Singapore.
3. Close contacts of Covid-19 patients
For close contacts of confirmed Covid-19 cases who were members of the same household, 285 samples from this group have been tested.
The results show that about 5 per cent of household members were eventually infected after the first person in the household was diagnosed.
Of this 5 per cent, half of them did not test positive for the infection during the time that they were quarantined and showed minimal to no symptoms. They were unaware that they were infected until after the serological tests.
Assoc Prof Ng Oon Tek, senior consultant at NCID, said that researchers are still analysing whether it can be conclusively said that the individuals in this group have no symptoms. This is because the responses from the risk questionnaires, which is another component of the study, are still being analysed.
The questionnaires were distributed to the participants for them to provide details about their exposure risks and past medical issues.
Assoc Prof Ng said that there is the possibility of what is called “recall bias”, where patients are unable to recall symptoms despite having them, for example. This needs to be taken into account when determining if these cases were asymptomatic.
Though the study found that the proportion of those who were eventually infected was low, Dr Chen said this does not mean that Covid-19 is not as infectious as it is said to be.
“The virus may also spread by other pathways outside of the household. For instance, we have observed the spread of the virus at social events and workplaces.”
He added that the research team is still investigating how Covid-19 spreads.
Agreeing, Assoc Prof Ng added that the household infection rate is measured in a setting where Covid-19 patients are moved out and household members are instructed to avoid physical interaction with one another.
Therefore, the infection rate is likely to be higher in household settings where these measures are not taken seriously.











