Study estimates 210,000 men have sex with men in S’pore, at risk of HIV
SINGAPORE — Researchers from the National University of Singapore (NUS) estimate that 210,000 men here have sex with other men, and they could face a concentrated epidemic of the human immunodeficiency virus (HIV).
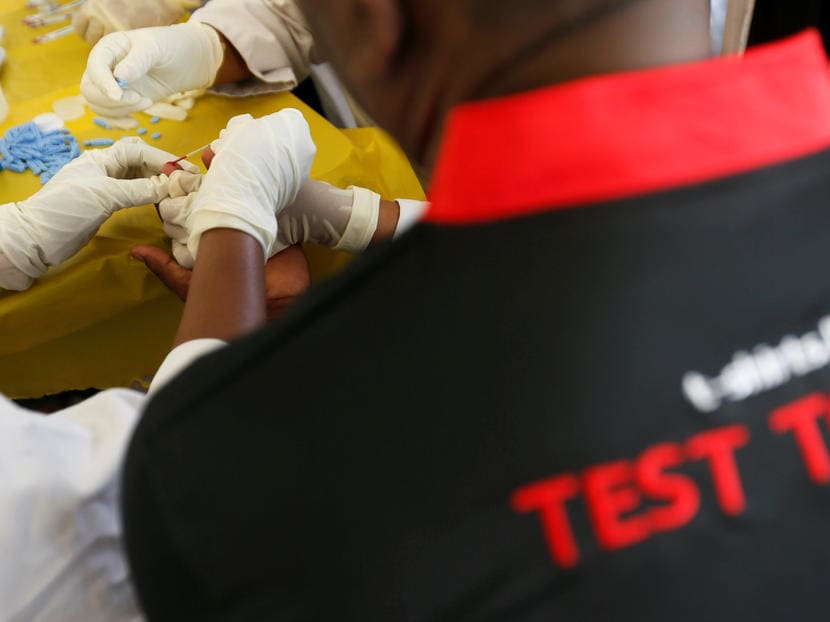
The HIV epidemic in Singapore is classified as low level, but researchers noted that it is “likely to be a concentrated epidemic among key populations such as men who have sex with men”.
SINGAPORE — Researchers from the National University of Singapore (NUS) estimate that 210,000 men here have sex with other men, and they could face a concentrated epidemic of the human immunodeficiency virus (HIV).The figure is more than double an earlier less rigorous estimate of 90,000 men.
The research, conducted at the Saw Swee Hock School of Public Health, marks the first time researchers have estimated the number of people in groups in Singapore who are at risk of HIV infection.
There are four key “hidden” population groups most likely to acquire and transmit HIV. They are estimated to be:
210,000 men who have sex with men
72,000 male clients of female sex workers
4,200 female sex workers
11,000 intravenous drug users
Published on May 9, the report provides the first empirical estimates of these groups living here. The study was funded by the Health Promotion Board and the Singapore Population Health Improvement Centre.
Singapore does not have a systematic approach to collecting data on the size of these key populations at risk of HIV. Not knowing these numbers prevents a gap in stamping out or treating HIV, which the report seeks to address.
The researchers — Mr Alvin Teo, Dr Kiesha Prem, Dr Mark Chen, Dr Adrian Roellin, Associate Professor Wong Mee Lian, Dr Hanh Hao La and Dr Alex Cook — said that the study will aid the effective planning of HIV care, treatment and support.
“The national size estimates of at-risk populations generated will help determine the magnitude and resources required for national HIV prevention and intervention efforts,” they said.
While the HIV epidemic here is now classified as low level, the researchers noted that it is “likely to be a concentrated epidemic among key populations such as men who have sex with men”.
A representative sample of 199 people in Singapore was surveyed from July to August 2017, when they were asked how many people they knew belonging to the hidden population groups.
The network scale-up method was then used to arrive at the numbers — where the population sizes of the at-risk groups were estimated from the respondents’ personal network size.
‘IMPORTANT’ FOR HIV PLANNING
The researchers pointed out the significance of the study method, having been done previously in various countries such as Ghana, Iran and Japan to estimate the size of hard-to-reach populations at risk of HIV.
“It yielded important information for individual country-level HIV prevention programme planning, monitoring and evaluation,” they said.
This is particularly significant with the estimate of 210,000 men who engage in homosexual sex — as the figure is more than double of a previous 90,000 estimate, based on guesstimates by community organisations.
The study also provides first-ever estimates of female sex workers and their clients.
Non-governmental organisations told TODAY that they welcomed the study, with the key findings providing a better understanding of the HIV situation in Singapore.
Ms Sumita Banerjee, general manager of advocacy group Action for Aids (AFA), said: “It helps us to understand the current gaps in our reach, and what is needed to fill that gap and the effectiveness of our current strategies.
“Based on these new estimates of the population sizes, under the current human and financial resources, we are able to reach only 25 to 30 per cent of these populations. We need to broaden our reach to effectively control and end HIV in Singapore.”
Responding to TODAY’s queries, a Health Promotion Board spokesperson said that the findings “should be interpreted with caution” due to limitations of the study such as its sample size, but acknowledged that the estimates “can be useful as one of the inputs for HIV prevention programme, planning, monitoring and evaluation”.
CONSIDERING SOCIAL STIGMA
Keeping in mind Singapore’s context, the researchers had factored in transmission error and barrier effect using social acceptance measures and demographics, to derive the estimates — extending previous work that “did not adequately accommodate such information”, they said.
Transmission error is where there is the possibility that members of the hidden population groups might not divulge membership to some of their contacts.
Additionally, not all respondents have an equal chance of interacting with members of the hidden populations, giving rise to what is termed the barrier effect.
Criminalisation of gay sex in Singapore may give rise to transmission error, the researchers said.
Section 377A in the penal code “amplifies discrimination against homosexual males, and therefore membership to this group may not always be known to their social contacts, resulting in transmission error,” they said.
Ms Vanessa Ho, executive director of sex workers’ rights group Project X, said that the transmission error for sex workers will be “substantial”, given society’s negative perception of them.
And for intravenous drug users, there is a barrier effect as “it is unlikely you will know someone who is one, unless you are a prison warden or a family member,” she said.
“Stigma, discrimination, criminalisation all work to drive these populations underground and make them reluctant to access healthcare services due to fear of identity exposure and risk of being criminalised, which is why there is a need to adjust for transmission error and barrier effect,” Ms Ho added.
“It is crucial that we understand why such a study is necessary in the first place, and also recognise that the fact that these populations are hidden means that much more resources need to be utilised to reach out to them.”











